Uveitis In India
About Uveitis ?
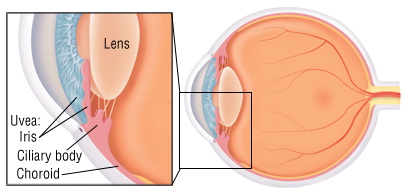
Uveitis (also known as iridocyclitis) is the inflammation of the uvea, the pigmented layer that lies between the inner retina and the outer fibrous layer composed of the sclera and cornea.The uvea consists of the middle layer of pigmented vascular structures of the eye and includes the iris, ciliary body, and choroid. Uveitis is an ophthalmic emergency and requires a thorough examination by an optometrist or ophthalmologist and urgent treatment to control the inflammation.
Classification
Uveitis is classified anatomically into anterior, intermediate, posterior, and panuveitic forms—based on the part of the eye primarily affected.Prior to the twentieth century, uveitis was typically referred to in English as "ophthalmia.
Anterior uveitis includes iridocyclitis and iritis. Iritis is the inflammation of the anterior chamber and iris. Iridocyclitis presents the same symptoms as iritis, but also includes inflammation in the ciliary body.Anywhere from two-thirds to 90% of uveitis cases are anterior in location. This condition can occur as a single episode and subside with proper treatment or may take on a recurrent or chronic nature.
intermediate uveitis, also known as pars planitis, consists of vitritis—which is inflammation of cells in the vitreous cavity, sometimes with snowbanking, or deposition of inflammatory material on the pars plana. There are also "snowballs," which are inflammatory cells in the vitreous.
Posterior uveitis or chorioretinitis is the inflammation of the retina and choroid.
Pan-uveitis is the inflammation of all layers of the uvea.
Causes
In anterior uveitis, no associated condition or syndrome is found in approximately one-half of cases. However, anterior uveitis is often one of the syndromes associated with HLA-B27. Presence this type of HLA allele has a relative risk of evolving this disease by approximately 15%.
Uveitis
Symptoms and signs
Redness of the eye.
Photophobia or sensitivity to light.
Irregular pupil.
Eye pain.
Floaters, which are dark spots that float in the visual field.
Signs of anterior uveitis include dilated ciliary vessels, presence of cells and flare in the anterior chamber, and keratic precipitates ("KP") on the posterior surface of the cornea. In severe inflammation there may be evidence of a hypopyon. Old episodes of uveitis are identified by pigment deposits on lens, KPs, and festooned pupil on dilation of pupil.
Diagnosis
Diagnosis includes dilated fundus examination to rule out posterior uveitis, which presents with white spots across the retina along with retinitis and vasculitis.